WHAT IS THE THYROID GLAND?
The usual test for thyroid disease are:
- Blood test (thyroid hormones, antibodies, markers), which examines the function of the gland.
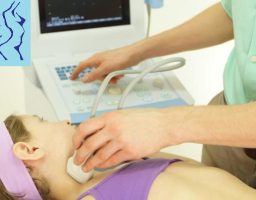
- Ultrasound, which diagnoses the morphology of the gland (size, presence of nodules, etc.)
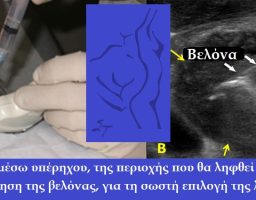
- FNA puncture (fine needle aspiration), which is done when there is a suspicion of malignancy.
This examination may be supplemented by scintigraphy or computed tomography, in those cases where it is deemed appropriate.
GOITRE

In thyroid disease goiter is any swelling of the thyroid, on the anatomical condition of the gland and not functional. May be accompanied by pro or hypofunction of the gland.
HYPOTHYROIDISM

Of the thyroid gland diseases, hypothyroidism is the pathological condition in which the level of thyroid hormones is low, that is, there is low secretion of thyroid hormones. Hypothyroidism is a more common condition in women, about 6: 1 and the symptoms are physical fatigue, mental laziness, cold intolerance, constipation, weight gain, dry skin, etc. Hypothyroidism is due in most cases today to thyroiditis, the most common of which is autoimmune chronic lymphocytic thyroiditis or Hashimoto’s disease. The body produces autoantibodies, which see the thyroid as a foreign body and try to destroy it.
Thyroid Disease – Hashimoto’s Thyroiditis

Of the thyroid gland diseases, Hashimoto’s thyroiditis is the most common inflammatory thyroid disease. It occurs when the patient’s antibodies attack their thyroid gland. The Hashimoto’s thyroiditis is most common in women aged 45-65 years, but can occur in patients of all ages.
Hashimoto’s symptoms:
- Constipation
- The skin is dry and thin
- Intolerance to cold
- Muscle aches
- Joint pains
- Increased bleeding during the days of the period, which lasts for more days
- Delayed psychosis, anxiety
How is it diagnosed?

- The gland is often hard, may be swollen or have several nodules
- Blood test to detect antibodies
- The TSH value is usually elevated
What is the treatment?
- Taking medication (hormone replacement) for those with hypothyroidism
- Surgical resection of the thyroid gland in patients whose swelling causes depressive symptoms or when the nodules swell
HYPERTHYROIDISM

Hyperthyroidism belongs to the diseases of the thyroid gland. It is a disorder of thyroid function, in which the gland overworks or causes an acceleration of metabolism. The thyroid may be morphologically normal or swollen (goiter). But it is usually increased in size and has nodules. The patient’s symptoms are weight loss that is not justified by exercise or food, palpitations and possibly arrhythmia, sweating, heat intolerance, nervousness, trembling, nausea which is often the reason why the patient goes to the doctor .
The most common cause of hyperthyroidism is Graves Basedow disease or diffuse toxic goiter. This is an autoimmune disease, meaning that the body produces autoantibodies that make the gland overactive. The second cause is nodular toxic goiter. That is, one or more nodules develop that result in the production of thyroid hormones in large quantities. The treatment of hyperthyroidism in the beginning can be pharmaceutical but in failure or in relapses the solution is the surgical removal of the thyroid.
Thyroid Diseases – Graves Disease

Graves’ disease also belongs to the thyroid gland diseases. It is an autoimmune disease that causes overproduction of thyroid hormones. A condition common in young women that can cause the thyroid to swell. Possible causes for Graves’ disease can be viral or bacterial infections as well as genetic ones.
What are the symptoms of Ms. Graves:
- Τrembling and muscule weakness
- Hair thinning or hair loss
- Increased appetite, diarrhea
- Irritability, anxiety, behavioral disorders, difficulty concentrating
- Intolerance to heat
- Weight loss without changing the diet
- Sleep Disorders
- Rapid heartbeat
- Obvious
How is the diagnosis made?

- Elevated T3 or T4 (thyroxine) values
- Low TSH value
- High antibody values
Treatment

Graves’ disease is treated with medication. In cases of patient adjustment but repeated recurrences, the solution is surgical removal of the thyroid.
THYROID CANCER

Among the thyroid gland diseases is thyroid cancer. It is the most common cancer of the endocrine glands and in fact with a large increase in its frequency in recent years, a disease which is now observed in children. Fortunately, in most cases it is curable. This of course depends on the type of cancer but also on the stage. There are four types of cancer: papillary, follicular, myeloid and regenerative carcinoma. The first two types are the most common (90-95%) which are curable, the myeloid (5%) which can be hereditary, ie patients carry a mutation in a gene (RET) and the last type, the anaplastic, which is very aggressive but fortunately is rare.
RISK FACTORS FOR THE APPEARANCE OF THYROID CANCER ARE:
- The female sex
- The history of goiter
- The family history of thyroid cancer
- Radiation exposure
DIAGNOSIS

Diagnosis is usually based on a good history, clinical examination, ultrasound, scintigraphy, and fine needle puncture (FNA). The ultrasound from specialized radiologists gives us valuable information and most of the time accurately diagnoses the existence of malignancy in both the thyroid and the lymph nodes, since with our mapping it indicates the suspected lymph nodes but also those that are infiltrated by malignancy. This is very important information, since this way we can accurately plan the operation we need to perform.
Excellent operation
It is very important that the initial operation is as perfect and complete as possible, because your prognosis depends on it. This means that if the operation is “incomplete” surgery (and unfortunately this is not uncommon):
- the ability to control the disease is impaired
- is likely to cause the need for additional surgery
- the chances of complications during reoperation increase
- potentially undermines survival.
TREATMENT

The main treatment for thyroid cancer is surgical removal of the thyroid, and depending on the type and stage, lymph node dissection may be needed. These are operations that require specialization, experience and delicate manipulations, so they must be performed by specialized surgeons who have experience in cancer surgery. This is why we tell our patients that if they come especially at an early stage, we can offer them a cure that is close to 100%.
Complementary therapy
Thyroid cancer surgery is usually supplemented with radioactive iodine, but it all depends on the quality of the surgery.
There are few cases where thyroid cancer does not respond to iodine, but in recent years new drugs have been discovered, with which we can help these patients as well.
CYST THYROLOGICAL RESOURCE

The thyroid gland cyst is a cyst with fluid in the front of the neck, just above the “Adam’s apple” and sometimes below.
They are cysts that sometimes remain after the development of the thyroid gland.
These cysts are present at birth and often occur in children.
About cysts:
- The bladder is usually a painless, soft, round mass on the front of the neck.
- It usually moves when the person swallows or sticks out their tongue.
- Surgical removal of the cysts helps prevent inflammation that may occur.
- They are often seen in preschool children or during adolescence.
How they are formed

During fetal development, the thyroid gland is located at the back of the tongue.
It then migrates to the throat, passing through the hyoid bone.
The hyoid bone is located at the root of the tongue in front of the neck.
As the thyroid gland descends, it forms a small channel called the thyroid gland.
This duct usually disappears when the thyroid gland reaches its final position in the neck. Sometimes part of the pore remains and leaves a cyst. It swells when fluid collects inside it.
Symptoms
In addition to its presence, sometimes mucus can leak through a small opening in the skin (fistula). If the bladder becomes infected, it may turn red and swell.
Some people with a thyroid gland may have difficulty swallowing or breathing. Sometimes people who have thyroglossic cysts may have a recurrent infection, excessive swelling, or symptoms of stress.
Surgery is the treatment when any of these symptoms occur.
Thyroid cysts may go unnoticed until they become inflamed.
Diagnosis
A cyst often occurs after an upper respiratory infection because it causes it to grow and become painful.
The symptoms of thyroid cysts can be attributed to other medical conditions and a detailed examination is necessary. Diagnostic tests may include any of the following:
- blood test
- ultrasound
- thyroid scintigraphy
- puncture and suction with a fine FNA needle
Once diagnosed, the doctor should refer the patient to a specialized thyroid surgeon.
Treatment
We thyroid and parathyroid surgeons usually remove the cysts of the thyroid gland to relieve the patient. Surgical removal allows further investigation. In rare cases, there may be cancer.
Antibiotics
Treating an inflamed bladder is treated with antibiotics, even if surgery is planned. Pre-surgery infection can make cyst removal more difficult and increase the chance of recurrence.
Do you have any question?
We know that there is a lot of information on our website and it can be difficult to assimilate it all. If you have any questions about our surgeon or the surgery you are about to undergo, contact with us and we will be happy to assist you.
COVID-19
Stay safe